If you or anyone in your family has these symptoms, call your doctor straight away or call 111. Say what the symptoms are. |
|
|
Babies and children
|
Teenagers and adults |
- You can also call Healthline free on 0800 611 116, 24 hours a day – even if you have already been seen by a health professional.
- If you have seen a doctor and gone home, but are still concerned, don't hesitate to call your doctor again or seek further medical advice. Sometimes meningitis can be hard to diagnose early on but it can get worse fast. Don’t be put off. Insist on immediate action.
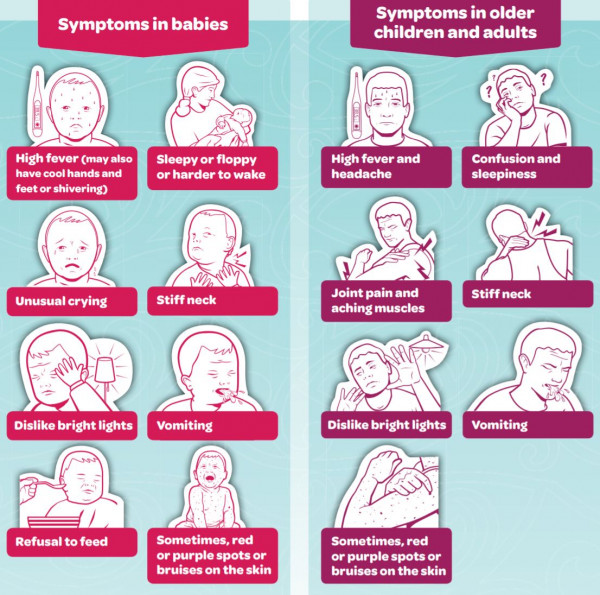
Image credit: Health Promotion Agency, NZ










