Self-management and self-management support
Managing your health conditions and getting support for your self-management
Key points about self-management and self-management support
- Self-management is taking charge of your own health and health-related decisions.
- It means having enough knowledge and confidence to be actively involved in what happens to you, and how your health conditions are treated or managed.
- Self-management involves understanding your conditions and the medicines you're taking and why. It involves working with your healthcare provider to set goals to achieve what you want for your own wellbeing and quality of life.
- It enables you to make informed choices about your health care and to live as well as you can with your health conditions.
- Find out about self-management and the support available to help you work towards improving your self-management skills.

Self-management is taking charge of your own health. It's especially important for people living with long-term conditions. To do this you need to be able to:
- find out more about your condition/s
- Learn new skills to help you manage your condition/s, such as pacing your activities if you have pain, or altering your diet if you develop diabetes.
- Make decisions about your own body.
- Plan what action you’re going to take.
- Develop a partnership with healthcare providers.
- Choose which of the available management options you are going to use, and which you chose not to use.
- Access resources.
- Solve any problems that arise.
Video: Self-management and self-management support
Here's a video that talks about what self-management is and how it can help you to improve your wellbeing. This video may take a few moments to load.
Self-management:
- puts you in control
- can improve your health – recognising a change in your symptoms and knowing what to do can stop things from getting worse
- saves time and money – you'll have less need for urgent appointments, which means less time off work/childcare
- leads to less anxiety – self-management can improve how you feel about your health. It can even feel better just to make a start on knowing more about your health and deciding what’s important to you.
Your healthcare provider should help you to self-manage by:
- listening
- pointing you towards reliable information, and discussing any questions
- using their experience and knowledge to help you weigh up options and decisions
- helping you set a goal and develop an action plan for how to achieve it
- being your healthcare partner, supporter and cheer leader
- reviewing things with you to help you stay on track, or when things change.
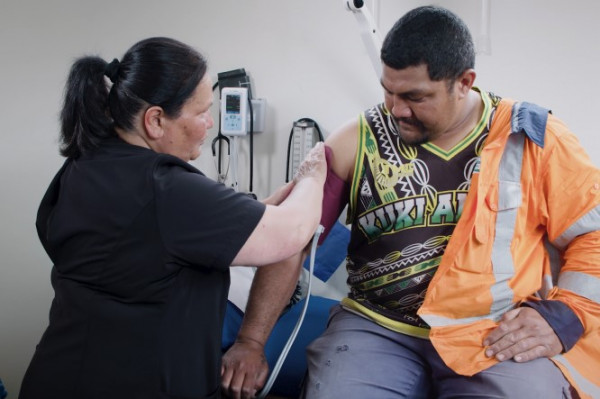
Image credit: Healthify He Puna Waiora
- Here! You’ve already started. Find out about your condition/s in the Health A – Z.
- A good thing to do next is to decide on your own health goals. Start with 1 goal in the area that matters the most to you. Seeing the benefit of that change will help you with the next goal. Remember that what’s important to you is something that will improve your quality of life. It might be directly related to a health condition (eg, diabetes or asthma) but it might be something else that’s getting in the way (eg, problems sleeping, anxiety about your health conditions, not being able to exercise because of your sore knees/hips). See making changes and goal setting for more information.
- Use the knowledge and skills you've gained from past life experience about what's important and what works for you.
- Use the support of friends and whānau.
- Make an appointment to see your healthcare provider. Tell them what you want, and ask them to work with you to develop a care plan for what you want to achieve. Read more about care planning and care plans.
- Keep a journal or diary.
- Use this template and instructions for writing down your goal and making an action plan for how to get there.
- The Centre for Clinical Interventions(external link) has many free online self-management workbooks, eg, perfectionism, procrastination and tolerating distress.
- Blood glucose monitoring at home for people with diabetes using medicines that need monitoring.
- Self-management apps.
- Health coaches.
- You might meet a health improvement practitioner (HIP) at your medical centre.
- Look up your local Primary Health Organisation website for resources, eg, Stanford self-management programmes.
- Programmes and courses for managing your health conditions.
- Support groups, national charities, patient groups.
- Pharmacists – community pharmacists have in-depth knowledge of medicines. They also have:
- ideas to help you take your medicines more easily
- reminder programmes
- time set aside for people with long-term conditions, so they can help you with questions about your medicines for free. It’s best to go in at a less busy time, but all you need to do is ask to speak with a pharmacist.
Healthify has a free wellbeing toolkit – Te Kete Haerenga – your journey to wellbeing kete. You can work through this yourself, with your whānau or download and take it with you to your appointment with your healthcare provider. It covers lots of areas that you may find challenging, especially if you have 1 or more long-term conditions. It guides you on making goals in areas like sleep, fatigue, pain and stress. It also has helpful diaries and tools to help you on your way.

Things to think about when you start out or continue with your self-management journey
- Priorities – if you have more than one long term condition, successfully managing one, can get in the way of getting a handle on another. For example you might want to get more exercise because you have high blood pressure, but you might also have osteoarthritis in your knees so walking hurts. Maybe instead you try aqua aerobics. You might need to try a few things, and change what you’re doing, before you get the right balance for you.
- Motivation – it’s hard to get motivated when you have a condition that isn’t going to go away completely. It can wear you down if it’s been going on for years. You might be able to borrow someone else’s motivation – meet up and work on your goals together or talk about shared experiences, or plan a reward to keep you going.
- Depression – people with long term conditions are at risk of depression. If you’re feeling sad, irritable or negative about yourself all the time you’ll likely need to get some help for this before you can self-manage your other conditions.
- Feeling powerless – it’s common to feel that you can’t make a difference to your health. But it’s usually true that you can make some difference to the way you feel. Talk with your friends, whānau or healthcare provider if you feel this way. Setting goals that are small and can be achieved will help you see that you can make a difference. This will be encouraging and you can build from there.
- Making too many changes at once – this can be overwhelming. Self-management is more likely to work well if you make one change and let that become part of your life before you move on to the next. While you’re deciding what you want to change think about it carefully. Making your goal a SMART one will make it more likely to you will be able to stick with your change. SMART stands for S (specific), M (measurable), A (achievable), R (relevant), T (time-bound). Read more about setting goals in the Te Kete Haerenga toolkit or on the care planning and care plans page.
- Complex information – if you have more than one healthcare provider and/or more than one long term condition you may get different information from different people. You may even get the opposite advice from different people. It’s hard to know who to listen to sometimes. If this happens you need assessment which takes into account all of your conditions and who you are as a person, proper follow up to change the plan if it affects another condition, and good co-ordination between providers. You might need to gently remind healthcare providers that this is what you need.
- Healthcare providers – your healthcare provider will be trying to do the best for you. They use their training, experience and guidelines based on research evidence to do this. The government and professional bodies have requirements your healthcare provider needs to follow. But sometimes they might be focusing on what they think is important to you. They may need a gentle reminder that the person who decides what is important for your health is you. You can take a support person to any appointment with you if this is difficult to say, or you could write it down first and read it out or give it to them to read.
- Finances – having a long term condition can affect both your income and your costs. Many people can get support from Work and Income. If you’re eligible for a community services card(external link) apply for one. Even if it doesn’t seem to make appointments cheaper, it can help when you’re away from home and with some other services, eg, X-rays in some parts of the country. Your medical centre may also have funding to help people with long-term conditions who are finding money is tight – your healthcare provider will most likely discuss this with you, but if not you can ask.
- Plan for setbacks – Think about what you will do if things don’t go well. Being prepared for setbacks can make them easier to handle. This includes having a sick day plan to follow if your daily activities and medicines are upset when you’re unwell. It’s good to have a plan so you already know what to do. It’s important to realise it’s only a temporary setback and you can pick up again when you’ve got better.
Apps reviewed by Healthify
You may find it useful to look at some Self-management and healthy living apps.
Motivation – how to get started and staying motivated(external link) Health Direct, Australia
Readiness for change(external link) University of Minnesota, US
Apps
Self-management and healthy living apps
References
- Lorig KR, Halsted PH, Holman R. Self-management education – history, definition, outcomes, and mechanisms(external link) Annals Behav Med 2003;26(1):1–7
- Gobeil-Lavoie AP, Chouinard MC, Danish A, et al. Characteristics of self-management among patients with complex health needs – a thematic analysis review(external link) BMJ Open 2019;9(5):e028344
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Emma Dunning, Clinical Editor and Advisor
Last reviewed:





