|
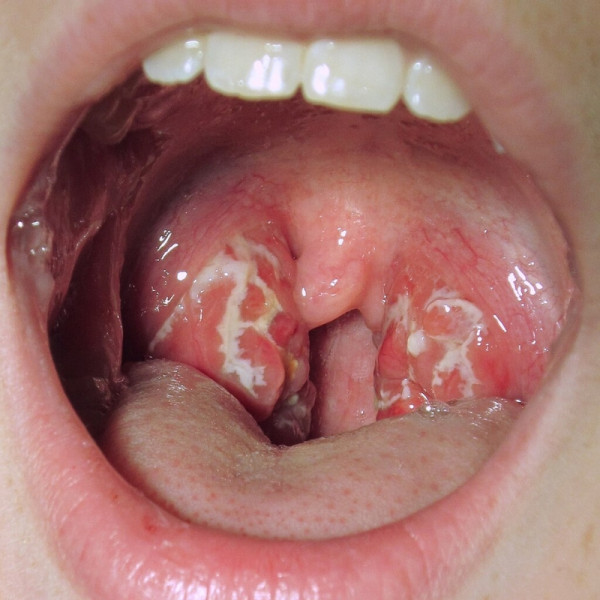
Reminder: If you have any respiratory symptoms (eg, a cough, sore throat, shortness of breath, head cold or loss of smell, with or without a fever) test for COVID-19 if you can. |
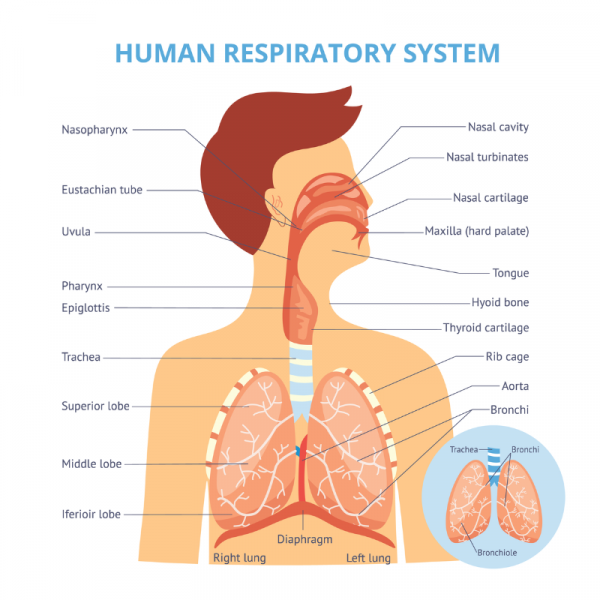
Respiratory tract infections (RTIs) are divided into 2 categories – upper and lower.
Lower RTIs, such as pneumonia, tend to be more serious than upper RTIs, such as colds or a sinus infection.
Most upper RTIs can be treated at home, but young children, older adults, pregnant people or people with long-term health conditions who get a lower RTI may need to see a healthcare provider.
You can reduce the spread of RTIs by:
- washing your hands
- covering your coughs and sneezes
- wearing a face mask
- getting vaccinations such as the COVID-19 and flu vaccines.
Practising health lifestyle habits such as eating well, avoiding smoking, getting plenty of sleep and exercising regularly will help you to stay well.