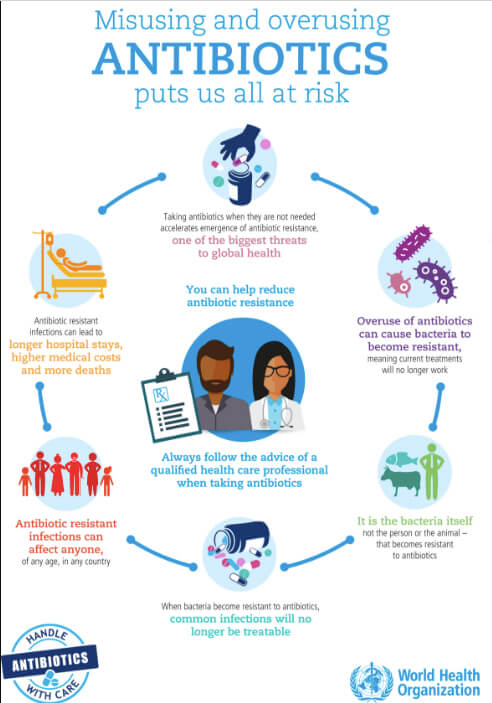
Antimicrobial resistance occurs when bacteria, viruses, fungi and parasites change over time and no longer respond to antimicrobial medicines. Infections become harder to treat and there is increasing risk of disease spreading, causing severe illness and death.
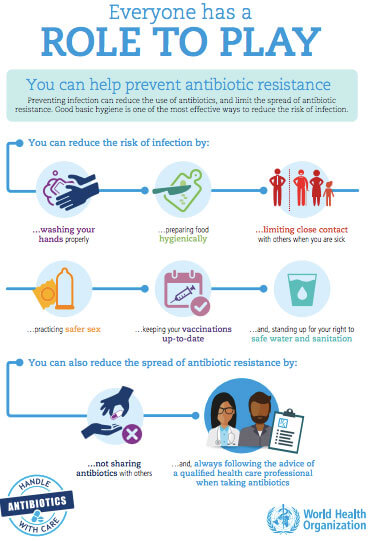
- Antimicrobial overuse increases the chance of some bacteria, viruses, fungi or parasites becoming resistant, which means when you next need antimicrobials they may no longer work to treat your infection.
- Resistant bacteria, viruses, fungi or parasites can multiply and spread to other people you have contact with, then these people can also develop antimicrobial-resistant infections.
What are antimicrobial medicines?
Antimicrobials include different groups of medicines, eg, antibiotics, antivirals, antifungals and antiparasitics.
- They're used to prevent and treat infections in humans, animals and plants.
- Antimicrobials are lifesaving medicines, but only if they work against the organism causing infection.
- Antibiotics are the most commonly prescribed antimicrobial.

Image credit: ACSQHC
Why is antimicrobial resistance a concern?
Antimicrobial resistance is a major concern because it means some infections will become more difficult, and sometimes impossible, to treat.
Antimicrobial resistance is a concern because:
- it can lead to "harder to treat" or "untreatable'" infections
- it can lead to longer stays in hospital
- it can increase the risk of infection associated with surgery and other life-saving procedures
- there aren't many new antimicrobials being created to treat resistant germs/bugs.
In Aotearoa New Zealand, the occurrence of antibiotic-resistant bacteria is increasing. Examples of antibiotic-resistant bacteria include:
- Methicillin-resistant Staphylococcus aureus (MRSA) – a group of bacteria (called Staphylococcus aureus) that are resistant to commonly used penicillin-like antibiotics. Read more about MRSA.
- Extended spectrum beta-lactamases (ESBL) – chemicals produced by some bacteria that prevent certain antibiotics from working. Read more about ESBL.
- Vancomycin-resistant enterococci (VRE) – a group of bacteria (called enterococci) that are resistant to the antibiotic vancomycin. Read more about VRE.