Scleroderma
Scleroderma and systemic sclerosis (SSc)
The name scleroderma literally means ‘hard skin’. The connective tissue of people with scleroderma has too much of a protein called collagen. Collagen is important to give connective tissue its strength, but too much collagen causes hardening and tightening of the affected area.
- Scleroderma is sometimes used as an umbrella term to refer to a group of rare, chronic conditions. Scleroderma can exist on its own, or may be the main part of a group of symptoms that make up a skin disease (eg, mixed connective tissue disease, lichen sclerosis, lipodermatosclerosis etc).
- Systemic sclerosis is a progressive autoimmune disease which causes scleroderma as well as affecting other connective tissues of the body (eg, muscles, joints, blood vessels and internal organs).

- Scleroderma can occur on its own or it may be part of another condition.
- There is no cure for scleroderma, but many treatments are available for specific symptoms and lifestyle measures can be helpful.
- It's not hereditary, so rarely occurs in more than 1 family member.
Scleroderma is the name given to hardening of the skin which is found in a number of skin and connective tissue diseases. Most commonly, scleroderma will appear as patches of thickened, tight skin across the body. There are 2 main types:
Localised scleroderma is sometimes called ‘morphoea’ (see the image below). It affects the skin and sometimes the deeper skin and muscle tissues directly beneath it. It more commonly starts in childhood and doesn't have associated disease in internal organs. Neither does it cause autoimmune antibodies (antibodies produced by your body that attack healthy cells instead of attacking bacteria or viruses). Read more about autoimmune diseases.
Linear scleroderma is thickened skin occurring in lines along the face, scalp, legs or arms. Occasionally it affects underlying bone and muscle. Linear scleroderma may improve after a few years, although it can affect the growth or movement of limbs.
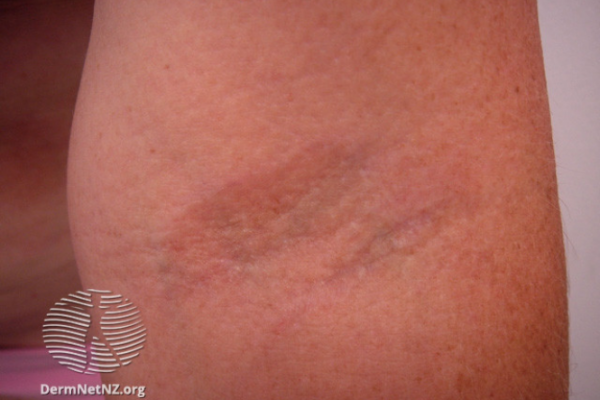
Image credit: Dermnet NZ
- Systemic sclerosis affects 5 times as many women as men, and the average age at diagnosis is around the 40s.
- It's rare, with prevalence varying from 30–500 cases per million.
- It's an autoimmune disease, therefore first degree family members (parent, full sibling, child) may be at a higher risk of being diagnosed with systemic sclerosis as well.
There are several types of systemic sclerosis, the most common types are outlined below.
Limited cutaneous systemic sclerosis (lcSSc) where you develop skin tightening over the face and below the elbows and knees and may also have gastroesophageal reflux disease. This type develops slowly and is often associated with pulmonary hypertension (high blood pressure in the blood vessels that supply the lungs – the pulmonary arteries).
CREST Syndrome is a very, very rare condition that includes a combination of the following signs:
- Calcinosis cutis (chalky calcium deposits under the skin).
- Raynaud's phenomenon (when the blood circulation in your fingers and toes is affected by cold).
- Esophageal dysmotility (where the tube carrying food and liquid from your mouth to your stomach doesn't work properly).
- Sclerodactyly (tightening and thickening of the skin on your fingers).
- Telangiestasias (dilated or broken blood vessels near the surface of the skin).
Diffuse cutaneous systemic sclerosis (dcSSc) affects various parts of the body including blood vessels, joints, the digestive system (oesophagus, stomach and bowel) and occasionally the lungs, heart and kidneys. Systemic scleroderma is more common in adults.
Systemic sclerosis sine scleroderma is a rare subtype without skin symptoms. People with this have internal organs affected by the conditions (as with dcSSc), Raynaud's phenomenon and auto-antibodies (as with SSc).
The symptoms vary greatly from person to person depending on what part of your body is involved and what the underlying disease may be. Symptoms can include any of the following:
- Thickening and hardening of the skin on the hands, arms and face.
- Stiffness and pain in the muscles and/or joints.
- Swelling of the hands and feet, especially in the morning.
- Thinning of the pads at the finger tips.
- Small, white, chalky lumps (calcium deposits) under the skin (calcinosis cutis).
- Indigestion or heartburn.
- Diarrhoea or constipation.
- Shortness of breath or reduced ability to exercise.
- Kidney problems and high blood pressure.
- Raynaud’s phenomenon where the fingers or toes turn white, then blue in the cold, and then red as blood flow returns. This is caused by narrowing of the blood vessels. Raynaud’s phenomenon can be experienced on its own, but most people with scleroderma will have symptoms of Raynaud's at some time and it is often one of the first symptoms to appear.
How do scleroderma and systemic sclerosis progress?
The experience of scleroderma and systemic sclerosis is different for everyone. For most people scleroderma starts slowly, affecting just a few parts of the body. It gradually gets worse at the affected site but usually becomes stable after a few years. Some people find their symptoms improve in summer but become worse in winter. Localised scleroderma doesn't develop into the systemic form.
People with systemic sclerosis can develop serious problems with other organs, so you may need to see a specialist if you have this condition.
As scleroderma is a feature of a number of conditions, it may take several appointments and tests to be certain of a diagnosis and it is important to tell the conditions apart.
There is no single test for these conditions, so it's recommended you see your doctor who can make a diagnosis based on your medical history and a physical examination. The characteristic thickening of the skin is often the key factor in making the diagnosis. However, tests can be helpful in establishing whether other parts of the body are involved, such as in systemic sclerosis. Tests could include:
- blood tests – to measure inflammation markers or auto-antibodies
- X-rays and CT (computed tomography) scans
- breathing tests – for pulmonary function
- heart scan
- skin biopsy, where a small piece of skin is removed and examined under a microscope.
At present there is no cure for scleroderma, but several treatments are available for specific symptoms. This is the same for systemic sclerosis but, depending on the areas that are affected, other treatment may be available. You will also be followed-up by your GP and other specialists.
Discuss your symptoms and treatment goals with your doctor. There's no easy way to predict what treatments will work for you. You may need to try several different treatments and medicines before finding the one that's right for you.
Here are some ways you can help yourself:
- Learn more about scleroderma: scleroderma differs from person to person but can be treated effectively, discuss your treatment options with your doctor and healthcare team.
- Exercise: one of the best things you can do is to follow a regular exercise regime. It will help to keep your joints flexible and improve blood flow. Your physiotherapist will design a programme to protect your skin and joints.
- Manage Raynaud’s phenomenon: avoid, where possible, exposure to cold and sudden temperature changes. Keep your whole body warm and protect your hands and feet with gloves and warm socks.
- Look after your skin: avoid strong detergents that can irritate your skin, keep your skin clean and well-lubricated to prevent dryness and infection. If you have particularly sensitive skin, soaps and creams may be available on prescription.
- Avoid smoking and nicotine products: tobacco smoking products contain harmful substances that damage skin and blood vessels. Nicotine replacement products (such as vaping) can also reduce the blood flow to the skin and delay skin healing.
- Manage stress: ensure you get sufficient rest and relaxation, and balance work and leisure. For support, talk to your health professionals, family and support groups.
- Healthy diet: including frequent small meals rather than the usual large meals, these may help if you have trouble with swallowing or heartburn.
Scleroderma New Zealand(external link) holds support meetings(external link) throughout Aotearoa New Zealand. They also provide information on financial support, hand therapists, podiatrists, mobility parking permits, home care support, rheumatologists, mental health support and more.
Scleroderma(external link) Arthritis NZ
Treatment and symptomatic management(external link) Patient Info, UK
Scleroderma(external link) NHS Choices, UK
What is scleroderma?(external link) Scleroderma Foundation, US
Support
Scleroderma NZ(external link)
Scleroderma Facebook support group(external link) NZ
References
- Scleroderma(external link) DermNet, NZ, 2010
- Systemic sclerosis(external link) DermNet, NZ, 2020
- Smoking and its effects on the skin(external link) DermNet, NZ, 2016
- Systemic sclerosis(external link) MSD Manuals, US, 2020
Apps
Nutrition, exercise and weight management apps
Skin care (dermatology) apps
Quit smoking apps
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Bryony Harrison, MBChB, BMedSci(Hons), DipPCEPE, Junior Doctor.
Last reviewed:
Page last updated:





