Treatment for ovarian cancer will depend on the type of cancer you have and the stage it is (how much it has spread). Treatment may involve a combination of surgery (to remove as much of the cancer as possible) and chemotherapy (to kill the remaining cancerous cells). Some people also choose to use complementary therapies. Palliative care is also available (specialised medical care to optimize your quality of life), and may be recommended if the cancer is very advanced.
Treatment options
Surgery
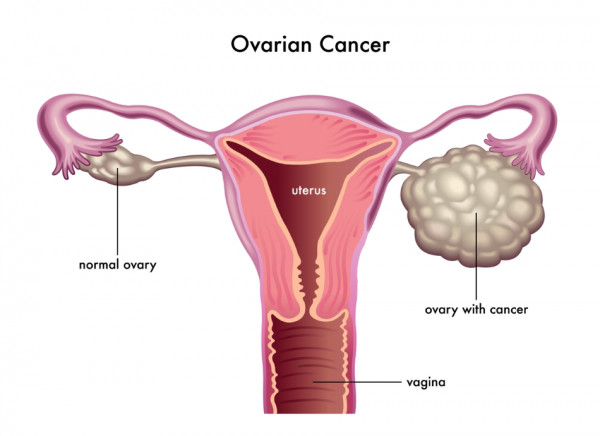
Most women with ovarian cancer will have surgery to remove as much of the cancer as possible. In germ cell tumours or in early stage ovarian cancer (stage 1), it may be possible to just remove the ovary. However, as the cancer can spread easily from the ovary to the uterus, fallopian tubes and omentum (membrane covering the organs in the abdomen and pelvis), often these organs are removed during the first surgery as well.
Surgery will not only treat the cancer by removing as much as possible, but it's also done to see if the cancer has spread. This is called staging.
Sometimes the cancer is too advanced for surgery to be possible. In this case, chemotherapy may be recommended as the first-line treatment.
Chemotherapy
Most women are also referred to a medical oncologist to discuss chemotherapy options. Even if all of the visible cancer has been removed, it is likely there are still cancer cells present (which are too small to be seen by the naked eye). Chemotherapy aims to kill these cells or shrink remaining masses, to prolong the time before the cancer grows again or causes symptoms. In a small number of women, chemotherapy can kill the cancer cells and prevent them from coming back (cure cancer).
Chemotherapy is usually given as a combination of different drugs. This improves the chances of killing the cancer cells but may also increase the damage to normal cells. Your specialists will recommend the best treatment for you and discuss these options with you.
Side effects of chemotherapy
Because the aim of chemotherapy is to kill cancer cells, these treatments may also damage normal cells. Cells that are rapidly dividing (eg, skin, hair and cells from the intestines) are particularly at risk of being damaged. This can cause hair to fall out and can also cause significant tiredness, a loss of appetite, nausea (feeling sick) or diarrhoea (runny poo). The team looking after you can help with many of these symptoms, so it's important to let them know what's happening.
Complementary and alternative therapies
The team providing your care will primarily be trained using conventional medical therapies. Some people may wish to use other therapies as well. Remember that it's your right to choose whatever therapy or therapies you choose, but also remember that your team is trying to look after you using the best information and evidence available. Some complementary and alternative therapies (including herbal or dietary supplements) will interfere with the treatment you receive, although many alternative therapies can be used alongside standard medical treatment. So it’s important to tell your team about anything else you are taking or doing.
Palliative care
Everybody starts their treatment for cancer in the hope that they will be cured and be able to get back to a normal life. Unfortunately, that isn’t the case for everyone. The palliative care team is trained to provide the best possible care to you and your whānau, to optimise your quality of life and provide support. They may be involved early-on in your care, to assist in managing symptoms from chemotherapy/surgery, or later on in your care to support you towards the end of your life. Read more about palliative care.
Who is in my treatment team?
Modern treatment of cancer is a team effort. You may have a lot of different people for different teams looking after you, but you should always have 1 or 2 main people you can contact if problems arise. Some health professionals that you may see include:
- Surgeons – who undertake any necessary surgery.
- Oncologists – who see you in clinic and look after the administration of chemotherapy.
- Radiologists or radiographers – who undertake and interpret the ultrasounds and other scans.
- Specialist nurses – your treatment is often supervised by nurses specialised in giving chemotherapy.
- Support staff – these range from the receptionist you see when you arrive for an appointment, to the orderly who collects your treatment, to the pharmacist who will be involved in your care.
- Dietitians – who can advise on the best foods to eat when recovering from surgery or when having chemotherapy.
- Social workers – who are able to inform you of available support services – especially if you're not able to work.
Apps reviewed by Healthify
You may find it useful to look at some Women's health apps and Mental health and wellbeing apps.