Breast lumps and changes
Key points about breast lumps and changes
- Most breast lumps are due to natural changes in your breasts during menstrual cycles, pregnancy, breastfeeding and ageing.
- However, sometimes a lump or change is found to be breast cancer.
- Being 'breast aware' means knowing what is normal for your breasts, and what changes to look and feel for so you can find them early.
- In fact, half of all breast cancers are found because someone noticed a change in their breast and showed their healthcare provider.
- Finding a breast lump or change early increases your chance of successful treatment if needed.

Breasts consist of:
- milk glands, which make breast milk and are made up of many milk sacs throughout your breastmilk ducts, which carry milk to your nipples
- fibrous tissue, which covers and supports your whole breast
- fatty tissue, which gives your breasts shape and size and supports the glands.
In your breasts, armpits and neck there are also collections of lymph nodes. These are small glands, each about the size of a pea, that drain your breast of lymph fluid, helping your body fight infection and disease. Your chest muscles and ribs lie beneath your breasts.
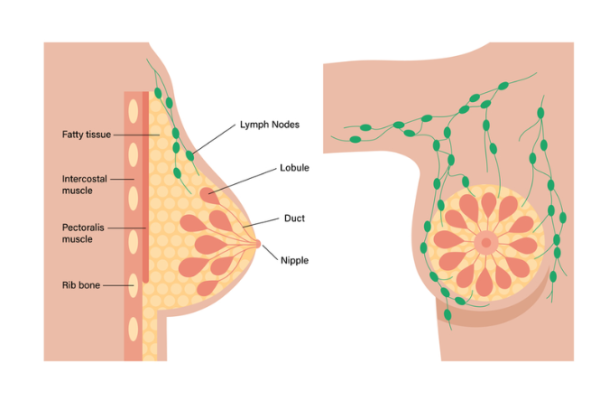
Image credit: Depositphotos
You may notice that your breasts are slightly different in shape or size or that one is slightly higher than the other – this is very common. If your breasts have always been like this, these differences are normal.
It's natural to have changes in your breasts during your menstrual cycle, pregnancy, breastfeeding or ageing. Read more about normal breast changes.
Most breast lumps aren’t cancer, but it’s important to get any breast lump checked so that breast cancer can be ruled out or diagnosed.
Non-cancerous (benign) breast lumps include lipomas, cysts and fibroadenomas. Read more about harmless breast lumps.
Breast awareness is knowing the normal look and feel of your breasts so that you can notice any changes quickly.
To be breast aware, you need to:
- know what's normal for your breasts
- know what changes to look and feel for
- book an appointment with your healthcare provider as soon as you notice any changes
- go to mammography screening if you are 45 to 69 years of age
- know your family history of cancer and advise your healthcare provider.
Look and feel for breast changes regularly, such as when dressing or showering, so that you get to know your breasts and how they change at different times of the month and as you get older. Read more about normal breast changes.
Video: Checked your breasts lately? We'll show you how.
(Breast Cancer Foundation NZ, 2015)
If you notice any change in how your breasts usually are, see your healthcare provider straight away. Examples of breast changes include:
- a new lump or thickening
- a change in breast shape or size
- pain in your breast
- puckering or dimpling of your skin
- any change in one nipple, such as a turned-in nipple or a discharge that occurs without squeezing
- a rash or reddening of the skin that appears only on your breast.
Although these changes don't necessarily mean you have breast cancer, any breast change should be checked by your healthcare provider. They will examine your breasts and may refer you for a scan (a mammogram or ultrasound). Read more about breast cancer.
Video: Be breast aware
This video includes examples of breast changes to look for.
It's common to have breast changes during your lifetime. Many of these changes are caused by hormones. Other breast changes can be caused by the normal ageing process.
Menstrual cycle – your breasts may feel more lumpy or tender at different times in your menstrual cycle. Before or during your menstrual periods, both of your breasts may feel swollen, tender or painful. You may also feel one or more lumps during this time because of extra fluid in your breasts. Wearing a supportive bra may be helpful. These changes usually go away by the end of your menstrual cycle.
Menopause – as you near menopause, your menstrual periods may come less frequently. Your hormone levels also change. This can make your breasts feel tender, even when you're not having your menstrual period. Your breasts may also feel more lumpy than they did before. They may also lose tissue and fat and become smaller. Read more about menopause.
Pregnancy – During pregnancy, your breasts may feel lumpy. This is usually because the glands that produce milk are increasing in number and getting larger in preparation for breastfeeding.
Breastfeeding – While breastfeeding, your breasts become full and firm with milk, then much softer after giving your baby a feed. It's not uncommon to have tender breasts. You may get a condition called mastitis. This happens when a milk duct becomes blocked and leads to inflammation. Mastitis causes the breast to look red and feel lumpy, warm, and tender. Read more about mastitis.
Hormone medications – If you are taking hormones (such as menopausal hormone therapy or birth control pills or injections) your breasts may become denser.
All breast lumps should be checked by your healthcare provider. Most breast lumps that develop before menopause are benign (not cancerous), but you need to get any lumps checked to rule out cancer.
Benign breast problems include pain, lumps or masses, infections, nipple discharge and skin changes. Common benign lumps include the following:
- Lipomas – these are lumps made up of fatty tissue and can be found just under your skin anywhere on your body.
- Cysts – these are fluid-filled sacs. You may have a single cyst or a number of different sized cysts. Your doctor may use a needle to remove the fluid in these.
- Fibroadenomas – these lumps are smooth, hard and movable, rather like a marble dropped into your breast tissue. They are common in women 18 to 30 years of age.
Read more about benign breast conditions(external link).
If you find a breast lump or change see your healthcare provider as soon as possible. They’ll examine your breasts and, if necessary, they’ll arrange further assessment, tests or scans.
Finding a breast lump or change early, and showing your healthcare provider, increases your chance of successful treatment if it’s needed.
There are things you can do to reduce your risk of breast cancer:
- Keep up with your free 2-yearly mammograms with BreastScreen Aotearoa if you qualify for these.
- Be breast aware – it’s important to check your breasts regularly even if you’re having regular mammograms.
- Have a healthy lifestyle, by:
- maintaining a healthy body weight, especially after menopause
- staying active with regular physical activity
- limiting alcohol consumption.
- Know your family history. Some types of breast cancer run in families so it’s important to know what’s happened in your family and advise your healthcare provider as extra screening may be recommended.
Breast awareness(external link) Breast Cancer Foundation, NZ
Breast screening(external link) Time to Screen, NZ
Breast lumps(external link) Breast Cancer Foundation, NZ
Benign breast conditions(external link) Breast Cancer Foundation, NZ
Breast lumps(external link) NHS, UK, 2023
Resources
Screening for breast cancer – joining BreastScreen Aotearoa(external link) HealthEd, NZ, 2024
Breast screening – information for women under 45 years of age(external link) HealthEd, NZ, 2024 also available in Thai(external link), Hindi(external link), Korean(external link), Japanese(external link), Chinese Simplified(external link)
Breast screening – information for women aged 70 years and over(external link) HealthEd, NZ, 2024
BreastScreeen Aotearoa – for Pacific women(external link) BreastScreen Aotearoa, NZ, 2019
Breast problems – swollen breasts(external link) La Leche League and Ministry of Health, NZ, 2018 also available in te reo Māori(external link), Samoan(external link), Tongan(external link), Niuean(external link)
Benign breast conditions – breast calcifications(external link) HealthEd, NZ, 2022
Benign breast conditions – fibroadenoma(external link) HealthEd, NZ, 2019
BreastScreen Aotearoa – NZSL version(external link)
Breast pain (mastalgia)(external link) HealthInfo, NZ, 2022
Apps
References
- Breast awareness – know your breasts(external link) Breast Cancer Foundation, NZ, 2025
- Understanding breast changes – a health guide for women(external link) National Cancer Institute, US, 2014
- Benign breast problems and conditions(external link)(external link) The American College of Obstetricians and Gynecologists, US, 2021
- Benign breast conditions(external link)(external link) Breast Cancer Foundation, NZ
- Phelan ST. ACOG guidelines at a glance – diagnosis and management of benign breast disorders(external link)(external link) Contemporary OB/GYN, 2017
- Breast awareness – risk factors(external link) Breast Cancer Foundation, NZ, 2025
BreastNet NZ(external link) by Breast Cancer Foundation, NZ, 2025
BreastScreen Aotearoa for health professionals(external link) Health New Zealand | Te Whatu Ora, NZ
Phelan ST. ACOG guidelines at a glance – diagnosis and management of benign breast disorders(external link) Contemporary OB/GYN, 2017
Brochures

Breast screening – information for women under 45 years of age HealthEd, NZ, 2024
Thai, Hindi, Korean, Japanese, Chinese Simplified
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Lisa Harris, Registered Nurse Prescriber in primary health; Cara Hafner, Registered Nurse and Lactation Consultant, NZ Breastfeeding Alliance, Christchurch
Last reviewed:







