An arrhythmia is an abnormal heartbeat caused by a problem with the electrical conducting system of your heart muscle.
We're aware of a problem when trying to use Zero Data to link to Healthify. Zero Data is managed by Health NZ and we are working with them to get this fixed.
Arrhythmia
Abnormal heartbeat
Key points about arrhythmia
- An arrhythmia is an abnormal heartbeat caused by a problem with the electrical conduction system of your heart muscle.
- Some types of arrhythmia are fairly common and don't cause any problems or need treatment.
- Other types are more serious and require treatment to reduce the risk of complications.
- This page focuses mostly on the more serious arrhythmias, there's another page on palpitations which focuses on the more common types (ectopic beats and sinus tachycardia).
Your heart has a natural pacemaker in the top right-hand corner. This is a group of heart muscle cells called the sinoatrial node. The sinoatrial node sends out regular electrical signals which travel down a conducting system, like electrical wires. The electrical signal makes your heart muscle pump. The top chambers (the atria) of your heart pump first, squirting blood into the bottom chambers which are called ventricles. Then the ventricles pump and send blood to your lungs and the rest of your body. You feel this as your heart beat or pulse. It's normally 60–100 beats per minute and has a regular rhythm.
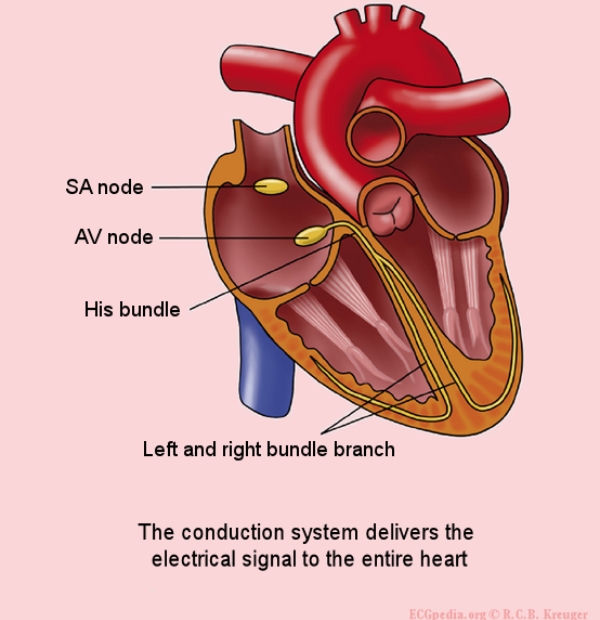
Image credit: Rob Kreuger, medical illustrator, AMC, The Netherlands, CC BY-SA 3.0(external link) via Wikimedia Commons
If the signal to pump comes from any other part of your heart, this system doesn’t work as well and your heart can beat too slowly, too fast or in an irregular rhythm. This can cause problems with the blood flow around your heart and around your body. A slow heartbeat is called a bradycardia, a fast heartbeat is called a tachycardia.
An arrhythmia can last for a second or a few minutes, or your heart can stay in an abnormal rhythm for days or permanently.
Some of the causes of electrical problems are:
- ischaemic heart disease (angina and heart attacks)
- heart valve disease
- cardiomyopathy
- congenital (being born with an electrical conduction problem)
- overactive thyroid (hyperthyroidism)
- high blood pressure
- some medicines.
- Palpitations – an awareness of your heart beating fast, slow or irregularly.
- Dizziness, faintness or collapse.
- Shortness of breath.
- Tiredness.
- Chest pain.
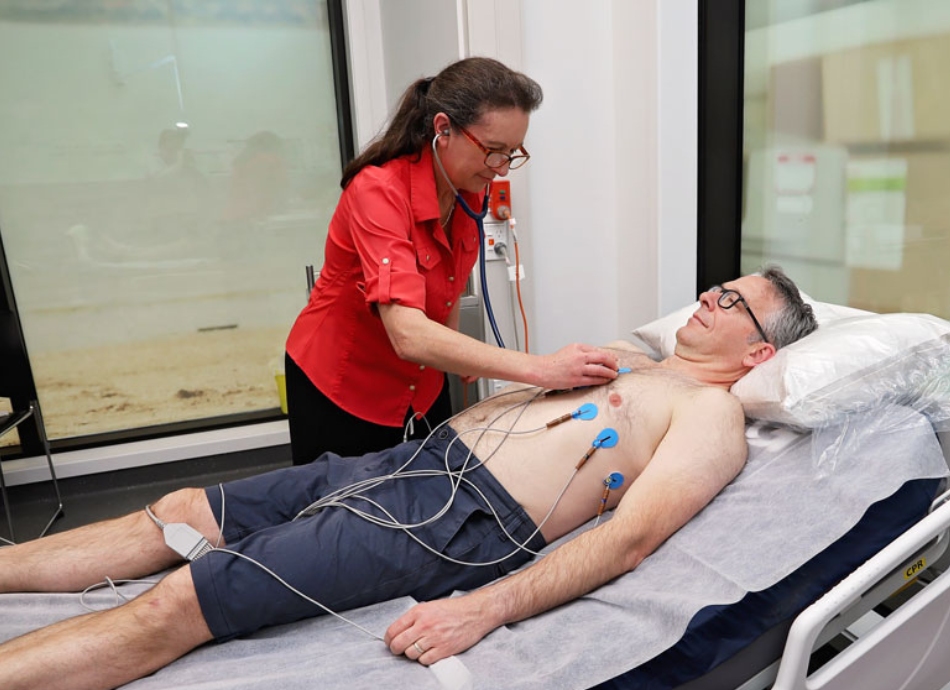
Your healthcare provider will ask questions about your symptoms and examine your chest and pulses. They will arrange an ECG, an electrical reading of your heart. Your GP or nurse practitioner will be able to diagnose and help you with most arrhythmias.
For some types, or if it's not clear what's happening, you might need to be referred to a cardiologist (heart specialist.) They can arrange a heart monitor which stays on your chest for at least 24 hours to find rhythm problems that come and go.
You may need other tests depending on the possible cause, eg, blood tests, echocardiogram or an electrophysiology study. Read more about heart tests.
Ectopic beats
These are extra heartbeats. The electrical signal comes from somewhere other than the sinoatrial node. We all get them and they are nearly always harmless. You don't normally notice them. You may notice them as a skipped beat or a stronger than usual beat in your chest if you're lying still in bed. Caffeine in tea or coffee, and alcohol may cause you to have more ectopic beats than usual.
Sinus tachycardia
Here, the heart rate from the sinoatrial node speeds up, eg, when you're exercising or have a fever. The rhythm is regular.
Supraventricular tachycardia (SVT)
A group of heart muscle cells or part of your electrical system in the top part of your heart (atria) start sending electrical signals faster than your sinoatrial node does. This makes your ventricles pump faster too, between 140 and 200 beats per minute (bpm). It sometimes lasts for a few minutes, it sometimes lasts for hours. This can happen to people in their twenties and thirties. It usually goes away by itself. Sometimes you can stop it by holding your breath (a Valsalva manoeuvre) or by plunging your face into a bowl of iced water. If it doesn’t go away after a few hours or if you feel very unwell, you can go to hospital where medicine or a shock can be used to get your heart rhythm back to normal.
Atrial fibrillation (AF)
AF is a fast irregular heart rhythm starting in the upper chambers (atria.) It can cause stroke or heart failure and often needs ongoing medication or a shock.
Atrial flutter
Atrial flutter is similar to atrial fibrillation. The atria beat at about 300 bpm but the ventricles are unable to beat that quickly and so beat at between 75 and 150 beats per minute.
Ventricular tachycardia
This is uncommon and serious. It starts in the lower chambers of the heart. There's a trigger of electrical signals somewhere in the ventricles which overrides the normal signals coming down from the sinoatrial node. The ventricles beat faster than normal (between 120 and 200 bpm). The rate in the atria is normal.
Ventricular fibrillation (VF)
This is a common cause of cardiac arrest and death. Electrical signals are triggered in many places in the ventricles so the muscle quivers and can't pump blood. It can only be fixed by a shock from a defibrillator given within a few minutes.
Heart block
This happens when the electrical signals are partially or fully blocked between the atria at the top of your heart and the ventricles at the bottom. The sinoatrial node in the right atrium sends signals at the normal rate but the rate the ventricles pump (heart rate) depends on how many signals get through to the ventricles:
- First-degree heart block means there's a slight delay in each signal, but each impulse does get through and your resting heart rate is normal. First degree heart block is only noticed on an ECG.
- Second-degree heart block means that some signals from the atria don’t get through to the ventricles. The ventricles can pump more slowly.
- Third-degree, or complete, heart block means that no signals are conducted through. The ventricles then pump at their own in-built rate of about 20-40 beats per minute. You have a very slow pulse.
Sick sinus syndrome
With this, the sinoatrial node becomes damaged. Your heart beats slowly or misses a few beats. Sometimes your heart changes between beating slowly for a while and then fast for a while.
If you have lots of ectopic beats or often have episodes of supraventricular tachycardia (SVT), avoiding alcohol, caffeine and drugs (eg, methamphetamine) can help.
Anxiety can make ectopic beats more noticeable, so breathing and relaxation techniques can help. You may find it useful to look at some Breathing apps, Anxiety management apps and Meditation and mindfulness apps.
If you're prescribed medicine it's important to continue taking it because the complications of untreated arrhythmias can be serious. If you have questions or side effects talk with your healthcare provider about making changes.
If you have collapsed or nearly collapsed because of an arrhythmia you won't be able to drive until it's been treated and you've had no symptoms for 3 months. Your healthcare provider will let you know about any driving or work restrictions due to other symptoms or procedures.
Some arrhythmias (eg, ectopic beats) don't need treatment.
Others can be treated with medicine, either just when they are happening or daily for prevention.
Sometimes cardioversion is used. This involves being given an anaesthetic to put you to sleep and your heart is given an electric shock. This stops the abnormal rhythm and your normal rhythm starts again.
Artificial pacemakers are used for complete heart block and sick sinus syndrome.
If you have episodes of life-threatening arrhythmias you can have an implantable cardioverter defibrillator (ICD) inserted under the skin of your chest, which gives an electrical shock when it detects an abnormal rhythm.
How the heart works(external link) Heart Foundation, NZ
Abnormal heart rhythms(external link) Patient Info, UK
Brochure
The following link provides further information about arrhythmias. Be aware that websites from other countries may contain information that differs from New Zealand recommendations.
Heart arrhythmias explained(external link) hearts4heart, Australia
References
- Palpitations(external link) Auckland region HealthPathways, NZ, 2023
- Abnormal heart rhythms(external link) Patient Info, UK, 2022
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Emma Dunning, Clinical Editor and Advisor
Last reviewed:





