How to use fluorouracil and imiquimod for non-melanoma skin cancer in a general practice setting(external link) BPAC, NZ, 2017
Actinic keratoses(external link) Dermnet, NZ, 2024
See our page Skin cancer for healthcare providers

You can now add Healthify as a preferred source on Google. Click here to see us when you search Google.

One spot is called an actinic keratosis. If you have more than 1, they're called actinic keratoses.
Actinic keratoses start as flat pink or grey scaly spots. They're rough to touch and grow into patches and get thicker. They can then look white or yellow. There are often more than 1 of them, and they can grow to join together. Sometimes they can be tender (sore to touch.)
Actinic keratoses are very common in places that get a lot of sun exposure, especially:
Actinic keratoses are precancerous. That is, some can develop into a type of non-melanoma skin cancer called a squamous cell carcinoma. The risk is small, but if you have many this can add up.
The images below show actinic keratoses on the back of a hand and on a forehead.
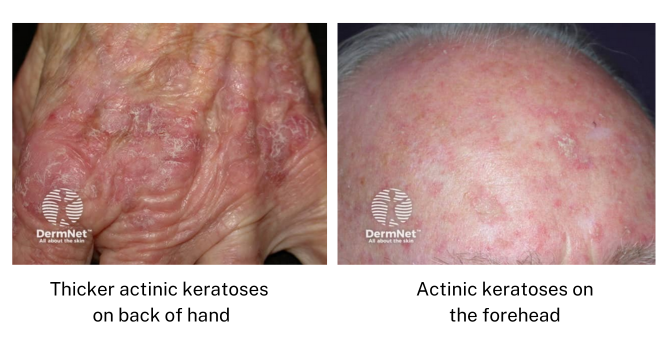
Image credit: DermNet NZ(external link)
Actinic keratoses are skin damage caused by years of exposure to ultraviolet (UVB) radiation found in sunlight. They're more common if:
They often start to appear when you're in your 60s.
Actinic keratoses have a typical appearance which can be diagnosed on examination by your healthcare provider. Sometimes they will use a dermoscope (a magnifying instrument). If they think you could have a squamous cell carcinoma (SCC) they might take a biopsy (a small sample to send to the laboratory). Read more about SCCs.
The aim of treatment is to remove the abnormal skin cells to prevent them becoming skin cancers. New skin then forms from deeper cells that have escaped sun damage. You may choose to have them treated because of how they look or where they are. Actinic keratoses are usually treated by your GP or nurse.
Treatment will depend on the size and number of the skin lesions and may include:
If actinic keratoses are widespread, it may not be practical to treat all of them. In that case, your healthcare provider will focus on the most thickened, tender or annoying ones. The thicker and tender ones are at greatest risk of progressing to skin cancer.
You may find it useful to look at some sun safety apps.
The best option for preventing actinic or solar keratoses from developing or getting worse is to protect your skin from the sun and UV rays.
Regularly check all your skin (from head to toe). If you see anything that is growing, bleeding or in any way changing, go and see your healthcare provider straight away.
Read more about skin checks.
Read more about sun safety.
Actinic keratoses(external link) NHS, UK
Actinic keratoses(external link) Molecheck, NZ
Efudix(external link) Medsafe, NZ
Actinic keratoses (also known as solar keratoses)(external link) British Association of Dermatologists, UK
How to use fluorouracil and imiquimod for non-melanoma skin cancer in a general practice setting(external link) BPAC, NZ, 2017
Actinic keratoses(external link) Dermnet, NZ, 2024
See our page Skin cancer for healthcare providers


Efudix Medsafe, NZ

Actinic keratoses (also known as solar keratoses)
British Association of Dermatologists, UK, 2020
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Emma Dunning, Clinical Editor and Advisor
Last reviewed: