You can now add Healthify as a preferred source on Google. Click here to see us when you search Google.
Pressure sores
Also called bed sores, pressure sores, pressure areas, pressure ulcers or a pressure injury
Key points about pressure sores
- Pressure sores are also known as pressure injuries, pressure ulcers, bed sores or pressure areas.
- They're caused by staying in one position for too long, such as if you’re sitting or lying for a long time and can’t move around.
- They usually form around bony areas of your body, such as your ankles, heels, hips and tailbone.
- The main complication of a pressure sore is an infected wound. See your healthcare provider immediately if you have any signs of infection.
- Pressure sores can take a long time to heal but there are things you can do to prevent them.
A pressure sore is an area of damage to your skin and the tissue underneath it that develops if you stay in one position for too long. An open wound can develop if the pressure on your skin isn’t relieved.
Having a pressure sore can have a huge impact on you and those caring for you. It can cause pain and discomfort and may result in a stay, or longer stay, in hospital, feelings of anger and blame possibly because of poor care, and reduced quality of life because of infection, delayed healing, altered body image and low mood.
Importantly, there are things you and your caregivers can do to prevent pressure sores. These include changing your position regularly, checking your skin every day, keeping your skin clean and dry, and eating a healthy diet.
If you have a pressure sore, it’s important to get it treated as soon as possible. If it’s not treated, you’re at risk of developing infections such as cellulitis, sepsis or bone and joint infections.
Prolonged pressure on an area of your skin stops the blood flow to that area. This cuts off the oxygen supply and causes skin cells to die and then your skin breaks down resulting in a pressure sore.
You’re at risk of a pressure sore if you’re unable to move around or change position easily and if you:
- spend long periods of time in bed, eg, because of a serious illness or disability, or after major surgery
- sit in a wheelchair or chair for long periods
- are an older person or frail, and have thin fragile skin
- have skin that’s often wet from sweat, urine (pee) or bowel movements (poo)
- have damp skin due to sweating
- can’t feel pain or pressure on an area of your skin, perhaps due to having had a stroke, diabetes, spinal cord injury or epidural anaesthesia.
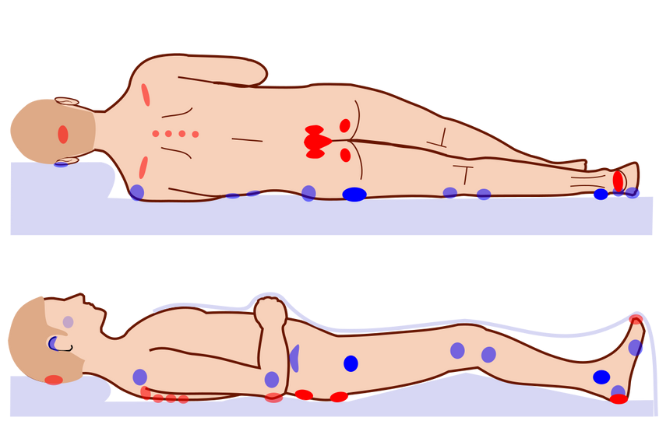
A pressure sore usually forms around bony parts of your body, such as your ankles, heels, hips and tailbone, as these areas take the weight of your body.
Being moved, or slipping down in bed, can also damage your skin or cause wounds in areas that are already damaged.
Pressure sores can develop in a few hours. The first sign is usually a discoloured area on your skin that doesn't turn white when you press on it. The injured skin may get progressively worse and eventually lead to an open wound.
Other symptoms include:
- pain, tenderness or itchiness of the affected area
- swelling
- reddened or discoloured skin – it can appear white or bruised
- blisters
- pus draining out from the affected area
- the skin being hotter or colder than other areas of your skin.
- any signs of infection such as fever and chills
- a sore that drains pus
- a smelly wound, or
- increased redness, temperature or swelling around a sore.
Your doctor or nurse will diagnose a pressure sore by examining your skin. They'll note how severe it is to decide what treatment is best for you. If they think it's infected, they may take a swab around your skin to find out the cause of the infection.
Depending on your health condition, you may need care from different healthcare professionals, such as your healthcare provider, a nurse specialising in wound care, an occupational therapist, a physiotherapist, a dietitian, a skin specialist or a plastic surgeon. Each of these are involved in different aspects of wound care.
Treatment may include:
- reducing pressure on the affected part of your skin by changing your position often and using equipment such as pressure-relieving mattresses and cushions
- medicines to control pain or itchiness
- cleaning the wound and covering it with dressings such as gel and foam-based dressings
- keeping your skin clean and dry
- maintaining good nutrition and hydration, as a poor diet can slow the healing of a pressure sore
- antibiotics if your wound is infected.
If you have a large, deep sore that doesn't heal properly, you may need surgery to remove damaged tissue.
Most pressure sores are preventable. It's much better to prevent pressure sores than to treat them.
Keep moving to relieve pressure
If you're in bed:
- change position every 2 or 3 hours – even a small shift in position can help
- use pillows to stop your knees and ankles touching each other, especially when lying on your side
- try to avoid creases in your bed linen
- if you're sitting up in bed, be aware that sliding down can cause injury to your bottom and heels
- ask for help if you need it.
If you're seated:
- relieve pressure by leaning forward or leaning side-to-side for a few minutes every half hour
- stand for a few minutes if you can
- go for a short walk if you can
- Ask your carer for help if you need it.
Other things you can do
Eat a healthy diet and drink plenty of fluids:
- A poor diet can affect the health of your skin and your immune system.
- Good hydration plays an important part in keeping your skin healthy and helps to repair injured skin.
- Being obese or having severe weight loss can increase the risk of getting pressure sores.
Keep your skin clean and dry:
- Keep your skin at the right moisture level, as damage is more likely to happen if your skin is either too dry or too moist.
- Ask your nurse or carer to help you with any incontinence or sweat. Immediately wash and dry skin and change clothing after any leakage of stool (poo) or urine (pee).
Check your skin at least once a day:
- Look and feel for changes such as redness, warmth, swelling, blisters, bruises, cracked, scraped or dry skin.
- Look closely at areas that are at high risk for pressure sores, such as your ankles, heels, hips and tailbone.
- You may need to ask someone to check difficult-to-see areas of your skin.
If you’re bed bound (unable to get out of bed), ask your healthcare provider about the use of heel and knee protectors or a pressure-relieving mattress.
Video: Shelley Roberts, Menzies Health Institute Qld, pressure injury prevention
Video: What are pressure injuries and how to prevent them – episode #67
Video: Pressure injuries part 2 – episode #69
The following links provide further information about pressure sores. Be aware that websites from other countries may have information that differs from New Zealand recommendations.
Pressure injury prevention and treatment(external link) New Zealand Spinal Trust
Pressure ulcer(external link) DermNet, NZ
Pressure sores – patient information(external link) BMJ Best Practice, UK
Skin care and pressure sores(external link) University of Washington, US
Brochures
How to prevent pressure injuries at home(external link) New Zealand Wound Care Society, Ministry of Health, Health Quality & Safety Commission & ACC, NZ
Available in the following languages: English(external link), Arabic(external link), Burmese(external link), Hindi(external link), Korean(external link), te reo Maori(external link), Punjabi(external link), Samoan(external link), Simplified Chinese(external link), Spanish(external link), Tagalog(external link), Tokelauan(external link), Tongan(external link), Traditional Chinese(external link), Tuvaluan(external link)
No pressure your skin matters(external link) New Zealand Wound Care Society, Ministry of Health, Health Quality & Safety Commission and ACC, NZ
References
- Preventing pressure injuries(external link) NZ Wound Care Society, NZ
- Pressure ulcer(external link) DermNet, NZ, 2023
- Helping prevent pressure injuries(external link) ACC, NZ
- The case for investment in – a quality improvement programme to reduce pressure injuries in New Zealand(external link) KPMG, NZ, 2015
Prevention and treatment of pressure ulcers/injuries: Clinical practice guideline – the international guideline fourth edition(external link) National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel & Pan Pacific Pressure Injury Alliance, 2025
How to classify and document pressure injury(external link) NZ Wound Care Society, HQSC, NZ, ACC & Ministry of Health, NZ, 2019
Guiding principles for pressure injury prevention and management in NZ(external link) HQSC, NZ, ACC & Ministry of Health, NZ, 2017
Pressure injury prevention(external link) Health Quality & Safety Commission NZ
Pressure injury in spinal cord injury – consensus statement(external link) ACC, NZ, 2021
Wound care – a guide to practice for healthcare professionals(external link) Ausmed Australia
Pan Pacific Pressure Injury Alliance(external link) Classification documents for different skin pigmentations
Brochures

New Zealand Wound Care Society, Ministry of Health, Health Quality & Safety Commission & ACC, NZ
Arabic, Burmese, English, Hindi, Korean, te reo Māori, Punjabi, Samoan, Simplified Chinese,Spanish, Tagalog, Tokelauan, Tongan, Traditional Chinese, Tuvaluan

New Zealand Wound Care Society, Ministry of Health, Health Quality & Safety Commission and ACC, NZ
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Jos Mehrtens, Registered Nurse, District Nursing Motueka
Last reviewed:





