Gallbladder surgery | Tangohanga kouawai
Also known as cholecystectomy (koh-luh-sis-TEK-tuh-me)
Key points about gallbladder surgery
- The gallbladder sits in the upper right part of your tummy.
- It stores bile which is a fluid made by the liver and helps breaks down fatty foods.
- Sometimes small stones can block the gallbladder and these stones are called gallstones. About 10 to 20% of adults in Aotearoa New Zealand are likely to have gallstones.
- You may have gallstones without having any symptoms but for some people gallstones can cause problems, eg, tummy pain, nausea (feeling sick) and yellowing of the skin (jaundice).
- Surgical removal of the gallbladder (tangohanga kouawai) is the most common way of treating troublesome gallstones. The procedure is called a cholecystectomy.

Your gallbladder is in the upper right part of your abdomen (tummy). Sometimes gallstones can form if the bile (digestive fluid) in your gallbladder hardens to form clumps. Bile flows from your gallbladder into your small intestine when you eat. If one or more gallstones moves out of your gallbladder, they can get stuck in the duct between the two. There they can cause problems and may have to be removed, usually along with your gallbladder.
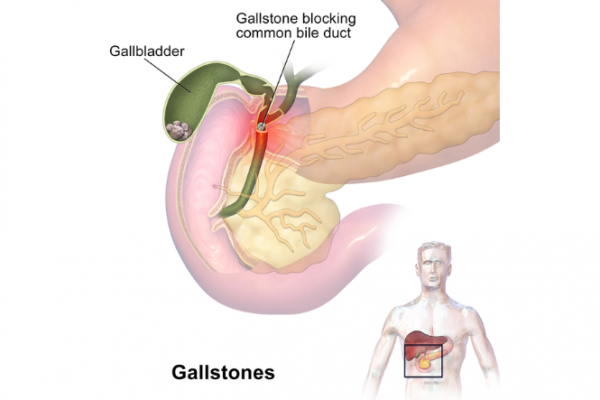
Image credit: Blausen.com via Wikimedia Commons
Gallbladder removal surgery is done by a surgeon in hospital. There are 2 main ways a surgeon can remove the gallbladder. For both procedures, you will be given a general anaesthetic (a medicine that puts you to sleep) so you don’t feel anything while the procedure is being done.
- Laparoscopic surgery: This is also called ‘keyhole’ surgery. This is the most common way of removing the gallbladder. The surgeon makes a few very small cuts on your tummy and into the small hole, they insert a thin tube containing a light and a tiny video camera. Next, the surgeon inserts special tools so they can remove the gallbladder. Keyhole surgery generally means a quicker recovery and less pain and a smaller scar than open surgery. Occasionally, if the keyhole surgery is more difficult than expected, your surgeon may need to move to an open surgery approach.
- Open surgery: This is where your surgeon will make a single, larger cut on your tummy so that they can take out your gallbladder. It's usually for people who can’t have keyhole surgery, eg, those with severe gallbladder disease or multiple previous abdominal operations.
The video below is about laparoscopic surgery for gallbladder removal.
Video: Laparoscopic NHS video
Gallstone removal surgery is a common procedure and you can live a healthy life without a gallbladder. Once it's been removed the bile from your liver makes its way directly out into you intestine and comes out in your poo. The bile ducts get larger and take on the role of storing bile.
Before you have gallbladder surgery, your healthcare team will do some tests (eg, blood tests) and check that the surgery is right for you. They will also decide if you need keyhole or open surgery. You will be told what you need to do to prepare for the surgery including when you need to stop eating and drinking before your operation and whether you need to stop taking any of your medicines.
Make sure you have someone who can take you home after your surgery.
Your surgeon will give you advice on what to do while you recover. Most people recover quickly from keyhole surgery and will usually be able to leave the hospital on the same day or the following day. It's best to rest for the next 2 weeks but you may need to rest for longer if you have a manual job. Do gentle exercise but don’t push yourself.
If you have open surgery, you will need to stay in hospital for a few days and it can take 4 to 6 weeks to get back to normal. Have a friend, whānau member or neighbour check up on you while you're recovering.
Possible side effects
Possible short-term side effects include:
- wound pain or swelling
- nausea (feeling sick)
- pain in your tummy
- bloating, wind or diarrhoea (runny poo).
These should get better in a few days. You could take paracetamol if needed for the pain. If you are very uncomfortable or these symptoms continue for more than a few days contact your healthcare provider.
Diet
It's best to have a healthy balanced diet after your surgery. If you have diarrhoea (runny poo) try eating high fibre foods (eg, vegetables and brown rice) to help firm up your poo. You may find it's best to stick to a low fat diet for a month or so while your body adjusts to not having a gallbladder. Your gallbladder is not essential for healthy digestion so most people find they don't have any ongoing digestive problems following their gallbladder removal.
Gallbladder removal surgery is usually a safe procedure but as with any procedure there are risks. Possible risks include:
- damage to the bile duct or liver
- bile leakage
- infection
- general surgery complications, eg, blood clots and pneumonia.
When to seek help
Contact your healthcare provider as soon as you can or call Heathline for advice (0800 611 116) if you experience any of the following symptoms after your operation:
- Ongoing discharge from your wound or worsening swelling or redness.
- A high temperature (fever).
- Dark urine and pale stools.
- Swollen tummy.
The following links provide further information about gallbladder surgery. Be aware that websites from other countries may have information that differs from New Zealand recommendations.
Gallbladder removal(external link) NHS, UK
Laparoscopic cholecystectomy(external link) HealthDirect, Australia
References
- Cholecystectomy (gallbladder removal(external link)) Mayo Clinic, US, 2023
- Do I need surgery for gallstones?(external link) WebMD, US, 2023
- Gallbladder removal (cholecystectomy)(external link) NHS 111 Wales, UK, 2024
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Michael Chu, General/HPB/Laparoscopic and Renal Transplant Surgeon
Last reviewed:





