The following information has been adapted from The Auckland Eye Manual(external link).
General description
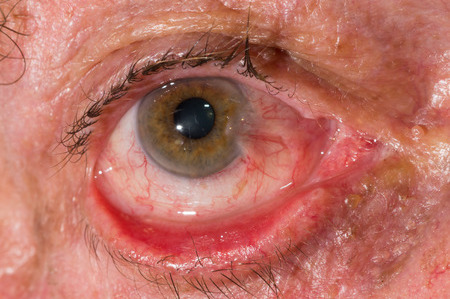
An ectropion is a positional problem of the eyelid in which the margin is rotated away from the globe. It is generally an involutional change related to laxity of the canthal tendons and lower lid retractor disinsertion. An ectropion can also be cicatricial related to skin shortage, mechanical from lid lumps or paralytic from seventh nerve palsy.
Symptoms
Commonly, patients have irritation from conjunctival thickening and drying. Watering relates to lid margin and punctal displacement along with secondary punctal stenosis.
Signs
There may be an elevated tear film (increased height of tear meniscus along the lower lid margin) and conjunctival inflammation in the region of the ectropion. Laxity of the medial or lateral canthal tendons is commonly seen. In cicatricial ectropion the skin can be generally shortened from sun damage or related to a scar. A paralytic ectropion will have the associated features of a facial palsy.
Slit lamp signs
Punctal stenosis is best seen on the slit lamp and this may also show maceration of the conjunctiva from prolonged exposure. In paralytic ectropion corneal drying, erosions and ulceration can occur from incomplete eyelid closure.
Immediate management
For corneal drying, regular lubricants are used (Lacrilube or Polyvisc ointment at night and artificial tear drops during the day). If there is any corneal ulceration, this must be managed with appropriate topical antibiotics. In cases of acute paralytic ectropion, the lower lid can be taped for support and Botox injected into the levator muscle to produce a temporary tarsorrhaphy.
Long-term management
In general, ectropion is well treated with surgery aimed at rectifying the underlying causes. This may include lid-tightening procedures, punctal opening and the addition of skin.
Referral guidelines
Most ectropions can be referred on a non-urgent basis unless there is concern regarding the health of the cornea.