COVID-19 treatment while you are in hospital
Key points about care in hospital when you have COVID-19
- COVID-19 is a viral infection that can affect your lungs and other body organs. It can cause minor to serious illness. There is no cure for the virus, but there are treatments that can help you feel better and decrease the chance of you becoming more seriously unwell.
- You have been admitted to hospital with COVID-19 so that you can be monitored and get help with your symptoms and any other medical problems.
- Being admitted to hospital with COVID-19 can be a worrying time, but knowing what to expect can help.

COVID-19 can affect many organs and systems of your body. You may need to be admitted to hospital for a variety of reasons, but most likely because you need regular monitoring and you're too unwell to fight off the virus at home and need specialist care.
There will be a number of hospital staff involved in your care such as doctors, nurses and physiotherapists. As these people work on rotation, you may not have the same person taking care of you every day. The medical team will review you daily to ensure you receive the highest quality and personalised care while you are in hospital.
There are social workers in hospitals who can help you access appropriate support and resources for your needs. Some hospitals will also have cultural support services available, eg, Māori, Pacific and Asian health services.
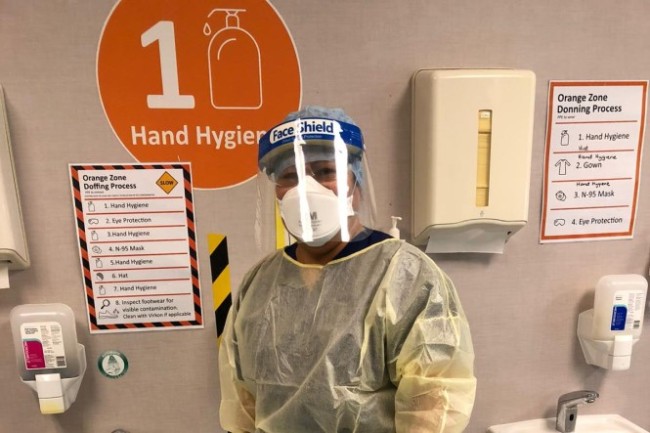
Image credit: Healthify He Puna Waiora
Stopping the spread of infection in hospital
Patient and staff safety is our priority, especially during the COVID-19 pandemic. To prevent the spread of the virus, we have a number of measures in place, such as isolation rooms and personal protective equipment (PPE clothing).
- All the people taking care of you will be wearing masks covering their mouth and nose, as well as gowns, gloves and visors or eye goggles.
- It may look a bit scary to start with, but this is to protect them from catching the COVID virus and passing it on to other patients.
- It may be hard to hear them when they talk to you, so let them know if you are finding it difficult to hear what they are saying.
- It may be hard to see their faces, but they will tell you their name and role as often as you need them to.
As part of your monitoring, there might be a computer or tablet in your room. This allows you to talk to staff without them coming in to see you. At times, your nurse might check on you through this, or your physiotherapist might do some breathing exercises with you without entering the room. This helps to limit the exposure of staff to COVID-19 by limiting the time they spend in your room where possible. It also helps them to prepare what they might need to bring into the room with them. Don't worry, if you need help they will always come in to see you.
Tests and monitoring symptoms
While you are in hospital your team will monitor your symptoms and your response to treatment. Your will have bloods tests and a chest X-ray on admission, and again as required. You may be asked to wear monitoring devices continuously to allow your team to monitor your breathing rate, heart rate, and oxygen saturation (how much oxygen is in your blood cells). It's important that these devices are kept on at all times even when you are asleep (they can be removed when you are using the bathroom).
If you are admitted to hospital for COVID-19, it may be that your lungs are affected and you require oxygen.
- Your medical team will decide on how to give you oxygen (see below for a description of the different oxygen devices) depending on your oxygen level; and this may change over time.
- You may have symptoms other than breathing problems which your team will discuss with you.
Devices to provide extra oxygen and/or pressure to keep your lungs functioning include the following:
Oxygen mask
Oxygen masks come in different types depending on your needs. This might be a mask that sits over your mouth and nose, delivering a small to medium amount of oxygen. The mask may have a small bag attached at the end to allow more oxygen in. It delivers a medium amount of oxygen.
Nasal cannula
These are small soft plastic prongs that sit in both nostrils, allowing the flow of oxygen into your nose. These might be small, low flow prongs that you don't notice or high flow devices that include warm humidified flow for comfort. The high flow device supports your breathing more, but can take some time to get used to. The advantage of this device is being able to eat and drink while using it. It delivers a small to medium amount of oxygen.
Non-invasive ventilation/CPAP/BiPAP
- CPAP is continuous positive airway pressure.
- BiPAP is bilevel positive airway pressure.
These devices involve using a tight-fitting mask to create a good seal to preserve the right amount of oxygen and pressure going into your lungs. It can feel like you have your head out of a car window on the motorway and can take some time to adjust to. This fast flow supports your breathing. Your team will inform you on how long you need to wear this mask and whether you can remove it for short periods, eg, for meals. It delivers a medium to high amount of oxygen.
Intubation
In very severe COVID illness, our critical care (ICU) team will consider placing a tube into your mouth and windpipe. A ventilator machine will provide oxygen to your lungs through this tube. You will not be awake. This is an invasive procedure, so the ICU team will talk to you and your family/whānau early on if they think you may need intubation. It delivers a high amount of oxygen.
There are a range of medicines to treat COVID-19 and its associated problems. They may be given to you based on how unwell you are and whether you have any other medical problems.
Getting medicines into your body
Some of the medicines you receive will be tablets and others will be given through an IV cannula (through your vein) into your blood. An IV cannula is a small, hollow, flexible plastic tube, which is usually inserted into the back of the hand or lower arm. You may feel some pain and discomfort when the cannula is being placed, but once the procedure has been completed the pain will stop. Please tell the person placing the IV cannula if you are uncomfortable or anxious.
|
Medicines to treat COVID-19 infection |
Medicines used to reduce inflammation in your lungs
|
Medicines used to slow down the virusAntivirals are medicines that reduce the amount of virus in your body that causes some infections such as COVID-19. They target specific parts of the virus to stop it from multiplying, helping to prevent severe illness. They are only useful when given within 5 days of the start of your COVID-19 illness.
|
Medicines used to reduce complications
|
New medicines and trials
|
Your regular medicines
You will often continue to take your usual medications. Your doctors will review them and tell you if they need to make any changes. If you are using any herbal medicines, natural supplements or Rongoā Māori, please do let us know. Some products may interact with medicines that you may need in hospital.
Unfortunately, you may not be able to have whānau or friends visit you in hospital while you are testing positive for COVID-19. Please check with your local hospital as visiting regulations may vary.
You should be able to stay in touch by phone or by computer or tablet if you have one in hospital with you. We understand that this is a difficult time for you to be away from your loved ones.
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Matthew Kelly, Infectious Diseases Physician, Health New Zealand | Te Whatu Ora, Capital, Coast and Hutt Valley
Last reviewed:





