Chickenpox | Mate koroputa hei
Key points about chickenpox
- Chickenpox (mate koroputa hei) is a common childhood illness that usually occurs between the ages of 2 and 10.
- It's caused by the varicella-zoster virus and isn't usually serious in tamariki.
- The main symptom is an itchy, blistering rash.
- Vaccination is free for children as part of the New Zealand immunisation schedule.
- Adults can still get if they haven't had chickenpox or haven't been vaccinated against it. It's often more severe in adults and is dangerous in pregnancy.

Chickenpox is caused by varicella-zoster virus, a virus from the herpes virus family.
The chickenpox virus is very contagious, which means it's very easy to catch. It's spread by sneezing and coughing, or by contact with the fluid inside chickenpox blisters. You can catch chickenpox from touching clothing or objects that have this fluid on them.
The time from catching the infection to seeing the rash (incubation period) for chickenpox is usually 14 to 16 days but it can range from 10 to 21 days.
You're infectious 2 days before the rash appears until all the blisters have dried up – when the spots are all scabbed over and dry. This usually takes 5 to 7 days.
While you're ill your body makes antibodies to the chickenpox virus. This means it's very unlikely you will catch chickenpox again. If you do, it will be mild.
You're at risk of getting chickenpox if you're exposed to the chickenpox virus and have never had chickenpox or haven’t had the chickenpox vaccine. In Aoteaora New Zealand, about 90% of people who are not vaccinated get chickenpox when they're children. If one child in your family gets chickenpox, it's very likely that other children (or anyone in your household who hasn't had it before) will get it also.
Chicken pox isn't common in tropical and subtropical countries. People moving to Aotearoa New Zealand from these countries aren't likely to have had chickenpox as children, so they're more likely to catch it as adults.
It takes 2 to 3 weeks for symptoms to appear after infection with the virus. A few days before the first spots appear, you or your child may have a fever, a headache, feel unwell or lose your appetite.
A few days later a red rash will appear:
- The rash normally starts on your face, stomach and back and spreads to other parts of your body. It may also cover your eyelids and mouth, and be up your nose and in your genital area.
- The rash spreads for 3 to 5 days.
- A few hours after each spot appears, it turns into a small blister filled with clear fluid called a vesicle.
- These vesicles are usually very itchy. The skin around them gets red.
- After a day or so, the vesicles burst, releasing the virus-containing fluid.
- Crusts or scabs form and take 1 to 2 weeks to fall off.
- The spots heal at different times, so your child may have the rash in several different stages at once.
Some people have mild chickenpox with fewer than 50 spots. Others have hundreds of spots and are very miserable.
Nausea, vomiting and tummy pain can also be caused by chickenpox. Teenagers and adults will often be more unwell than children.
| Chickenpox is most infectious from 2 days before the rash is present until after scabs have formed on all the sores and no new sores develop. This usually 5 to 7 days. Children with chickenpox need to stay home from school and early childhood centres during this time. |
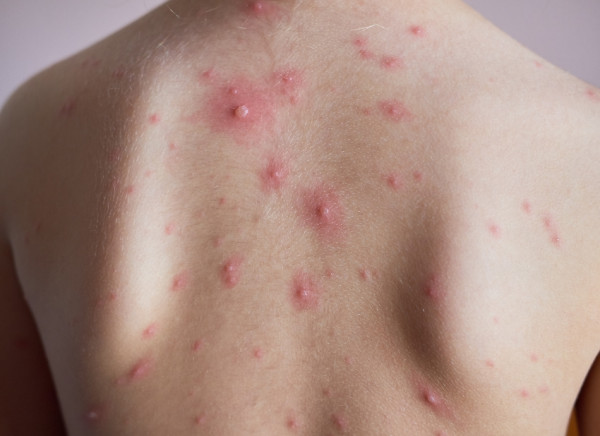
Image credit: Canva
There are risks for the pregnant person and unborn baby if chickenpox occurs during pregnancy. The mother can suffer more severe illness, complications and even death.
The highest risk for the pēpi is in the first 20 weeks of pregnancy. Infants exposed to chickenpox before birth are at risk of congenital varicella syndrome and may have skin scarring, eye, limb and brain problems and developmental delay.
Maternal chickenpox around the time of delivery can infect your newborn baby. Newborn babies who get chickenpox may have severe disease that can result in death. If you’re pregnant and think you have been exposed to chickenpox, call your GP or lead maternity carer as soon as possible as there is treatment available.
If you're planning a pregnancy and haven't had chickenpox, ask your midwife or healthcare provider whether you need to be vaccinated against chickenpox first. This is especially important if you didn't spend your childhood in Aotearoa New Zealand. If you have a chickenpox vaccination, you should avoid getting pregnant for at least 4 weeks afterwards.
Pregnant people shouldn't be given the chickenpox vaccine because its safety for the unborn baby has not yet been proven. However, no harmful effects have been reported when pregnant women have been vaccinated before they knew they were pregnant.
- Applying a soothing cream (emollient) such as Alpha Keri or fatty cream may help soothe the itch. Calamine lotion, the white lotion which was used for chickenpox in the past, is no longer recommended because it can dry the skin too much.
- To prevent dehydration, make sure your child has plenty of clear fluids (water, thin soup or ice blocks – avoid fruit juice if they have vesicles in their mouth). Don't worry if they don't eat much while they're sick – this will be fine for a day or two.
- Trim their fingernails and make sure their hands and fingernails are kept clean.
- Use mittens or clean socks on their hands to decrease scratching, especially overnight.
- Dress your child in loose-fitting clothing and change their sheets daily.
- Try a lukewarm bath. Don't use soap as this will irritate their skin. Add 2 cups ground oatmeal or half a cup of baking soda to make the bath more soothing. Pat their skin dry after bathing, don't rub.
Medicines
- Paracetamol – this can help reduce pain and headaches. Make sure you measure children's doses accurately and follow the directions given on the bottle or packaging. See our paracetamol dose calculator for help.
- Antihistamines – if you or your child can't sleep because of the itching, an antihistamine medication may help. Ask your healthcare provider or pharmacist to help you choose.
- Antibiotics – chickenpox is caused by a virus, so antibiotics aren't used to treat it. However, if the spots look like they may have become infected with bacteria, your doctor or nurse practitioner may prescribe an antibiotic to treat the infection. To prevent infection, it's important not to scratch the sores.
You should avoid the following medications
- Aspirin – never give your child or young person aspirin as this may increase the risk of Reye syndrome, which is a rare and serious illness.
- Ibuprofen (Nurofen, Brufen, Fenpaed) – the use of ibuprofen may be associated with more severe skin and soft tissue infections after chickenpox (particularly necrotising fasciitis, a rare infection of the deeper layers of skin).
For most people, treatment aims to lessen the symptoms and support your body's immune system to do the rest. Follow the advice in the self-care section above.
For people over the age of 12 who haven't had chickenpox before and haven't been vaccinated, it's possible to treat it with an antiviral called aciclovir. This has to be prescribed by a doctor or nurse practitioner and needs to be started within 24 hours of the rash appearing. It can reduce the length of fever.
People with severe immune system problems (eg, people with leukaemia, pregnant people and babies less than a week old) who are at risk of severe complications or death can be given chickenpox antibodies. This is a blood product called varicella immune globulin and is very scarce. This is why people in these groups need to contact their healthcare professional immediately if they've been in contact with someone who has chickenpox.
If you've had chickenpox or shingles in the past 6 months, think about donating blood to make varicella immune globulin. Find out more about donating blood after having chickenpox or shingles.
For most children, chickenpox is a mild disease that doesn't cause any lasting problems. About 1 in 20 healthy children develop a bacterial skin infection from chickenpox, usually from scratching the spots. This may need to be treated with antibiotics. Untreated bacterial skin infections can sometimes lead to more serious infections in your lungs or bloodstream infection (septicaemia).
Sometimes scars can be left where the spots have been. These often look like dips in your skin.
However, there are rare serious complications of chickenpox:
- Pneumonia/pneumonitis – lung infection or inflammation.
- Brain inflammation – encephalitis or Reye syndrome.
- Arthritis – inflammation of your joints.
- Hepatitis – liver inflammation.
When to get help
Contact your medical centre if the person with chickenpox develops any worrying symptoms such as:
- very high fever
- nausea and vomiting
- sensitivity to light
- stiff neck
- confusion
- severe headache
- any difficulty breathing
- drowsy and hard to wake
- fits (seizures)
- unable to drink due to severe rash in the mouth
- severe rash that looks infected or a rash that bruises or bleeds into the skin
- becoming generally more and more unwell.
If you're concerned, call Healthline on freephone 0800 611 116 for advice or contact your medical centre.
Chickenpox is spread through the air, when an infected person coughs or sneezes, or through contact with the fluid in the blisters. Chickenpox is infectious 2 days before the rash appears until all the blisters have dried up.
The person with chickenpox shouldn't go to work, school or preschool until all the blisters have dried up. This usually takes 5 to 7 days. Wash your hands often and after tending to your child and keep coughs and sneezes covered.
For children who haven't been very sick with chickenpox, staying at home can be difficult. But for some children and adults, chickenpox can be a very serious illness, so it's best to do all you can to stop it spreading. If you get chickenpox as an adult, it’s also important that you stay at home during the infectious period.
Vaccination against chickenpox is free for:
- children at 15 months of age
- children turning 11 years of age if they haven't had chickenpox or been vaccinated against it earlier.
Complications of chickenpox are rare but can be very serious or even fatal, especially for pregnant people and newborn babies.
People with a weakened immune system are at high risk of catching the virus, but may not be able to have the vaccination themselves, so it's recommended that close contacts of these people be vaccinated. The vaccine is funded for certain high-risk people and/or their close contacts. Read more about the chickenpox vaccine.
Video: Chickenpox – disease and vaccination New Zealand
Most people make a full recovery within 3 weeks. You may be left with a few skin-coloured scars, which are often dips in your skin.
You now have antibodies to chickenpox and you're very unlikely to catch it again.
The varicella virus stays in your body, in the nerve roots of your spine. Later in life the virus can wake up and cause a rash in the area of skin served by that nerve. This is called shingles or herpes zoster.
The following links provide more information on chickenpox.
Chickenpox(external link) Health New Zealand | Te Whatu Ora
Chickenpox (varicella)(external link) The Immunisation Advisory Centre, NZ
Brochures
Immunise against chickenpox(external link) Ministry of Health, NZ te reo Māori(external link)
Keeping skin healthy(external link) Health Literacy NZ
Infectious diseases(external link) HealthEd, NZ
References
- Varicella (chickenpox)(external link) Immunisation Handbook, NZ, 2020
- Chickenpox(external link) DermNet, NZ
Clinical guidelines and best practice guidance
From: Auckland Regional HealthPathways(external link)
Pre-conception consultation:
- If a woman has not had chickenpox infection, check varicella serology.
- If non-immune, offer vaccination (not subsidised).
- Advise to avoid pregnancy for 4 weeks after vaccination.
Chickenpox clinical practice guidelines(external link) Royal Children's Hospital Melbourne, Australia, 2021
Immunoglobulin administration(external link) Auckland Regional HealthPathway
Chickenpox in pregnancy(external link) Green-top Guideline No. 13, Royal College O&G, UK, 2015
Credits: Healthify editorial team. Healthify is brought to you by Health Navigator Charitable Trust.
Reviewed by: Dr Emma Dunning, Clinical Editor and Advisor
Last reviewed:





