Pityriasis rosea is a common skin rash. You usually get it between the ages of 10 and 35 years, and it most often happens in winter. It lasts 6 to 10 weeks then goes away without needing treatment.
Pityriasis rosea usually starts with a single pink or red round or oval patch on your chest, back or tummy. This is called a herald patch. It’s about 2 to 5cm across. The centre of the patch might be scaly, and it might have a red rim.
The image below shows a person with pityriasis rosea and the herald patch can be seen as an oval patch under the collarbone on the right of the image.
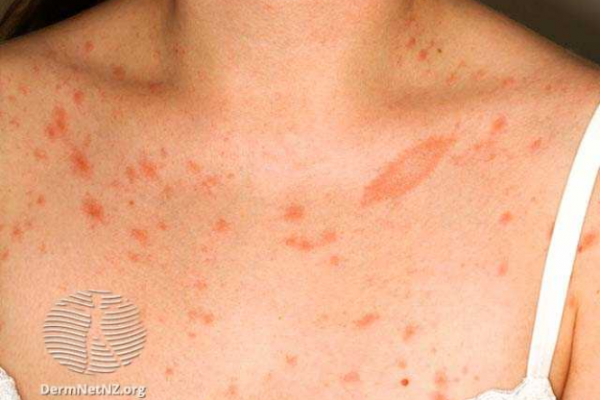 Image credit: DermNet NZ
Image credit: DermNet NZ
About 7 to 14 days later, lots of pink or red flaky patches appear all at once. The rash occurs mostly on your upper body and arms. The patches can follow the lines of your ribs, so this is sometimes called a Christmas tree pattern. You can sometimes get patches on your legs too. You don’t usually get it on the palms of your hands or the soles of your feet. If you’re pregnant, have dark skin or are younger the rash can be bumpier or even look like blisters. As the rash clears up, the patches of skin can look lighter or darker than usual, but this usually disappears over a few more months. It doesn't leave scars.
Video: Pityriasis rosea
This video may take a few moments to load.
(Family Doctor, Australia, 2015)






